Searching for private clinic providing any of the below?
Welcome to GB Clinics in Oxford, where comprehensive care meets innovation to empower your health journey at every stage of life. Your wellness is our priority.
LEARN MORE BELOW ⬇️
Explore Our
Injection Services
Steroid/Cortisone Injections
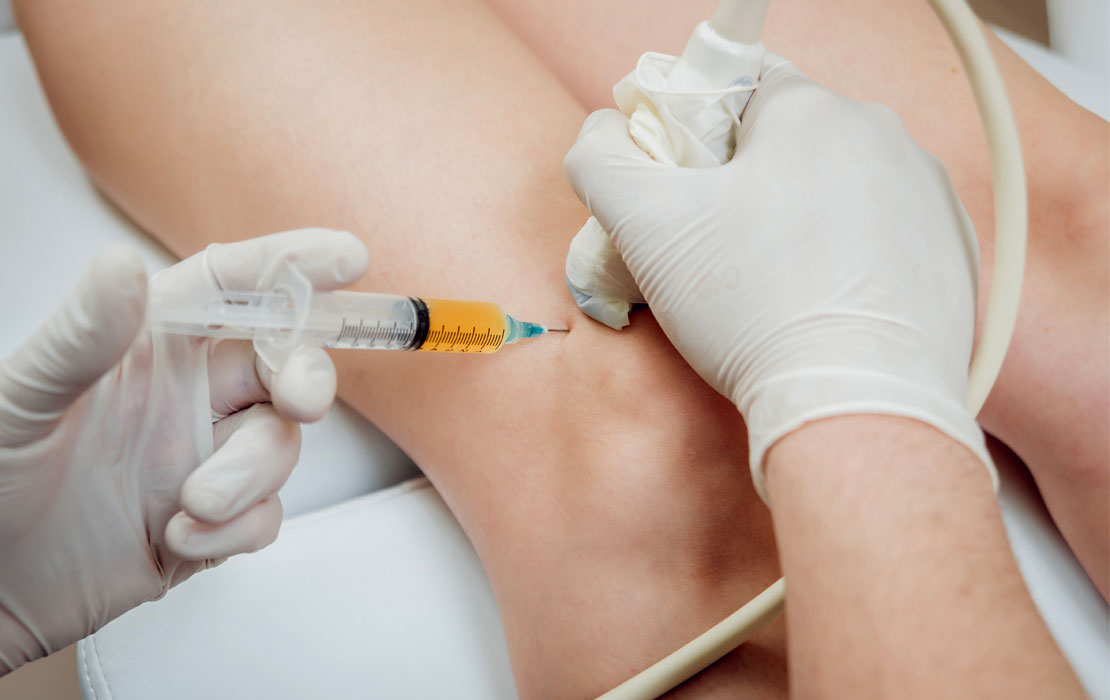
(We also provide Joint Aspiration as required.)
Why an Ultrasound-Guided Corticosteroid Injection is better:
Greater accuracy – the needle is placed exactly at the target area.
Better pain relief – medication reaches the correct tissue.
Safer – avoids nerves, blood vessels, and other sensitive structures.
Fewer complications – lower risk of misplacement or injury.
Often more effective – may reduce the need for repeat injections.
Real-time guidance – the clinician can see the needle and tissue throughout the procedure.
In short, ultrasound guidance makes the injection more precise, safer, and more effective than a “blind” injection.
Ultrasound-Guided
Corticosteroid Injection

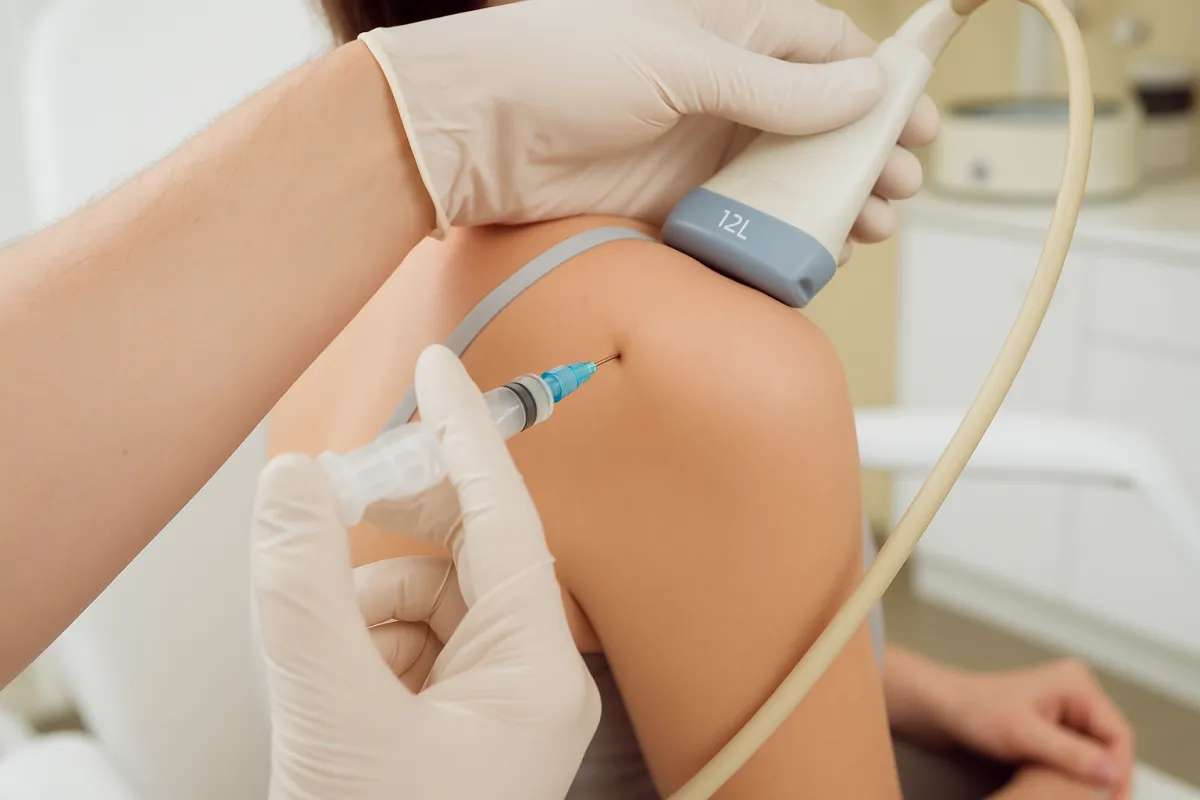

Joint Injections
Joint injections offer a safe and effective way to manage joint pain by delivering treatment directly to the source of discomfort. They can help reduce inflammation, improve movement, and allow you to return to everyday activities with greater comfort.
Hyaluronic Acid (HA) joint injections:
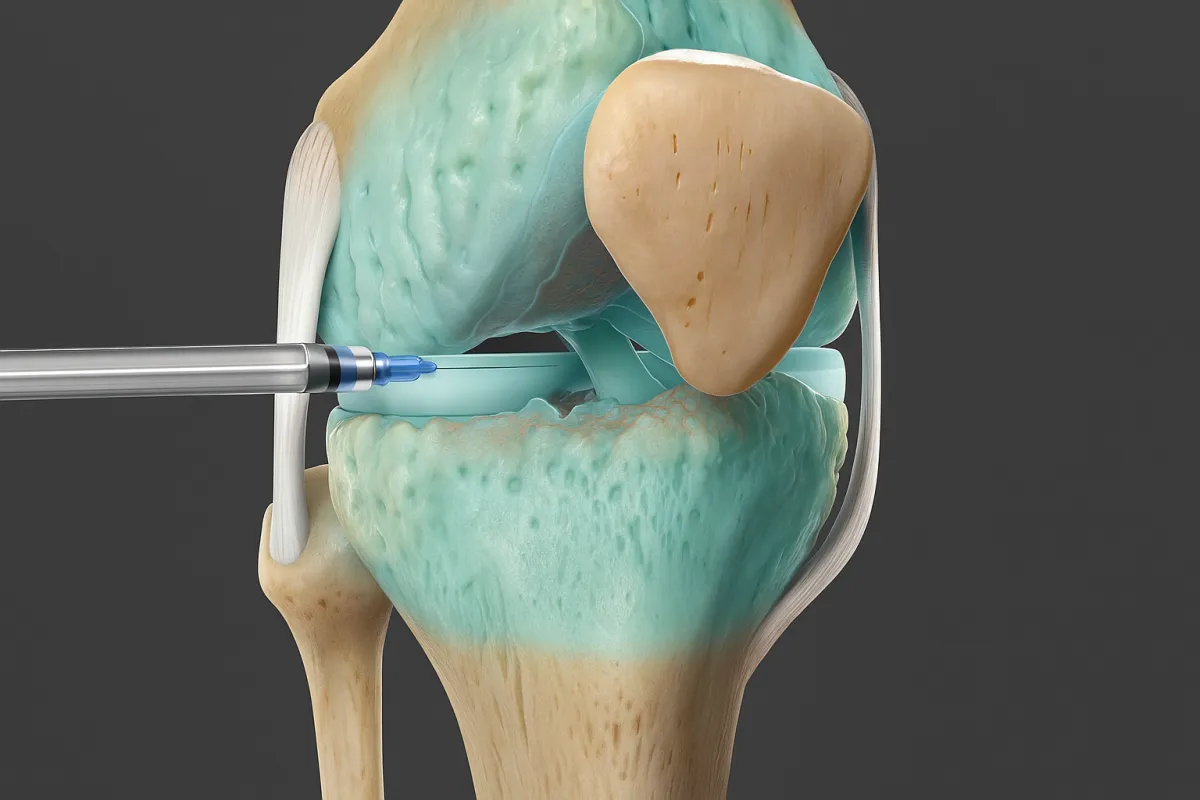
Hyaluronic acid injections are a minimally invasive treatment used to help reduce joint pain and stiffness, most commonly in osteoarthritis.
They involve injecting hyaluronic acid, a naturally occurring substance found in healthy joint fluid, directly into the joint. This helps improve lubrication and shock absorption, allowing the joint to move more smoothly and with less pain.
Hyaluronic acid injections are often used when symptoms persist despite exercise, physiotherapy, or simple pain relief, and can provide symptom relief for several months without using steroids.
Ostenil
Type: Hyaluronic acid (HA) injection
Used for: Osteoarthritis, most commonly the knee
What it does: Improves joint lubrication, reduces pain and stiffness, and supports smoother movement
Key point: Helps restore the joint’s natural cushioning and may provide relief for several months
Biolevox
Type: Hyaluronic acid (HA) injection
Used for: Osteoarthritis and degenerative joint pain
What it does: Reduces friction within the joint, easing pain and improving mobility
Key point: A non-steroid “gel injection” option, suitable when longer-term joint support is desired
Durolane
Type: Hyaluronic acid (HA) injection
Used for: Osteoarthritis (most commonly the knee)
What it does: Improves joint lubrication and shock absorption
Key point: Usually given as a single injection with long-lasting effect (often several months)
Sinogel
Type: Hyaluronic acid (HA) injection
Used for: Joint pain and osteoarthritis
What it does: Reduces friction in the joint, easing pain and stiffness
Key point: May be given as a single injection or short course, depending on the joint
Cingal
Type: Combination injection (Hyaluronic acid + corticosteroid)
Used for: Painful osteoarthritis with active inflammation
What it does:
Steroid → fast pain and inflammation relief
Hyaluronic acid → longer-term joint lubrication
Key point: Designed to give both quick and sustained relief

Arthrosamid injections
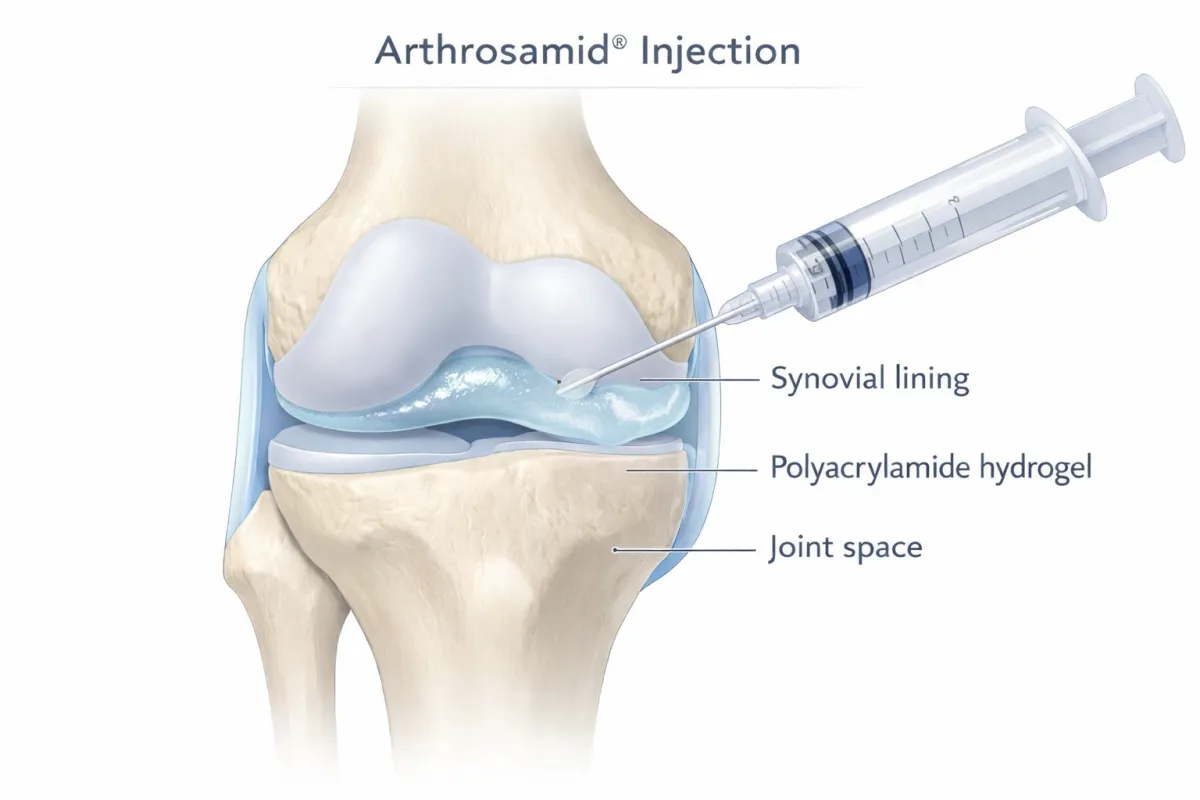
Arthrosamid injection is a minimally invasive, image-guided treatment used to manage chronic knee osteoarthritis pain.
What it is:
A single intra-articular injection of polyacrylamide hydrogel (a synthetic, non-biologic material) delivered into the knee joint under ultrasound guidance.
It does not contain hyaluronic acid or steroid.
What it does:
Integrates into the synovial lining of the joint
Acts as a long-lasting cushion and shock absorber
Improves joint biomechanics and load distribution
Reduces pain by decreasing mechanical stress and irritation within the joint
Unlike steroid injections, it does not primarily target inflammation, and unlike hyaluronic acid, it is not gradually broken down over months.
What it’s used for:
- Chronic knee osteoarthritis pain
- Persistent symptoms despite physiotherapy, weight management, or simple analgesia.
- Patients seeking a longer-lasting option than steroid or hyaluronic acid injections.
- Individuals wanting to delay or avoid surgical intervention.
The procedure is quick, typically performed under ultrasound guidance, and most patients resume normal activity shortly afterwards.
Pain relief may develop gradually over weeks and can last 1–2 years or longer from a single injection.

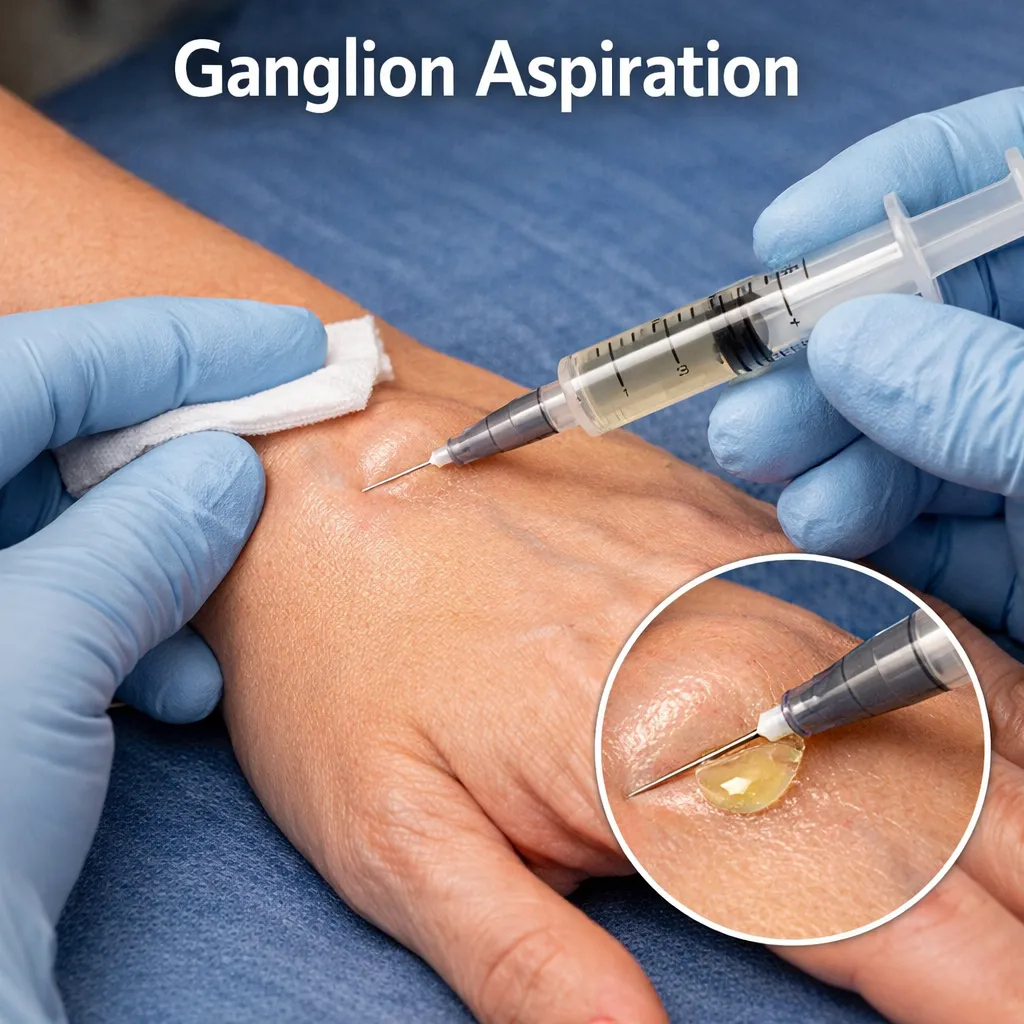
Ganglion Aspiration

Ganglion Aspiration is a simple, minimally invasive procedure used to treat a ganglion cyst—a fluid-filled lump that commonly appears around the wrist or hand (and sometimes the ankle or foot).
It involves inserting a fine needle into the cyst to draw out the thick, jelly-like fluid, helping to reduce the size of the lump and relieve symptoms.
What it’s for:
Reduces pain, pressure, or discomfort
Improves movement and function
Minimises visible swelling
Avoids surgery in many cases
The procedure is quick, usually well tolerated, and often performed in a clinical setting with little to no downtime.
Shoulder Hydrodistension for Frozen Shoulder
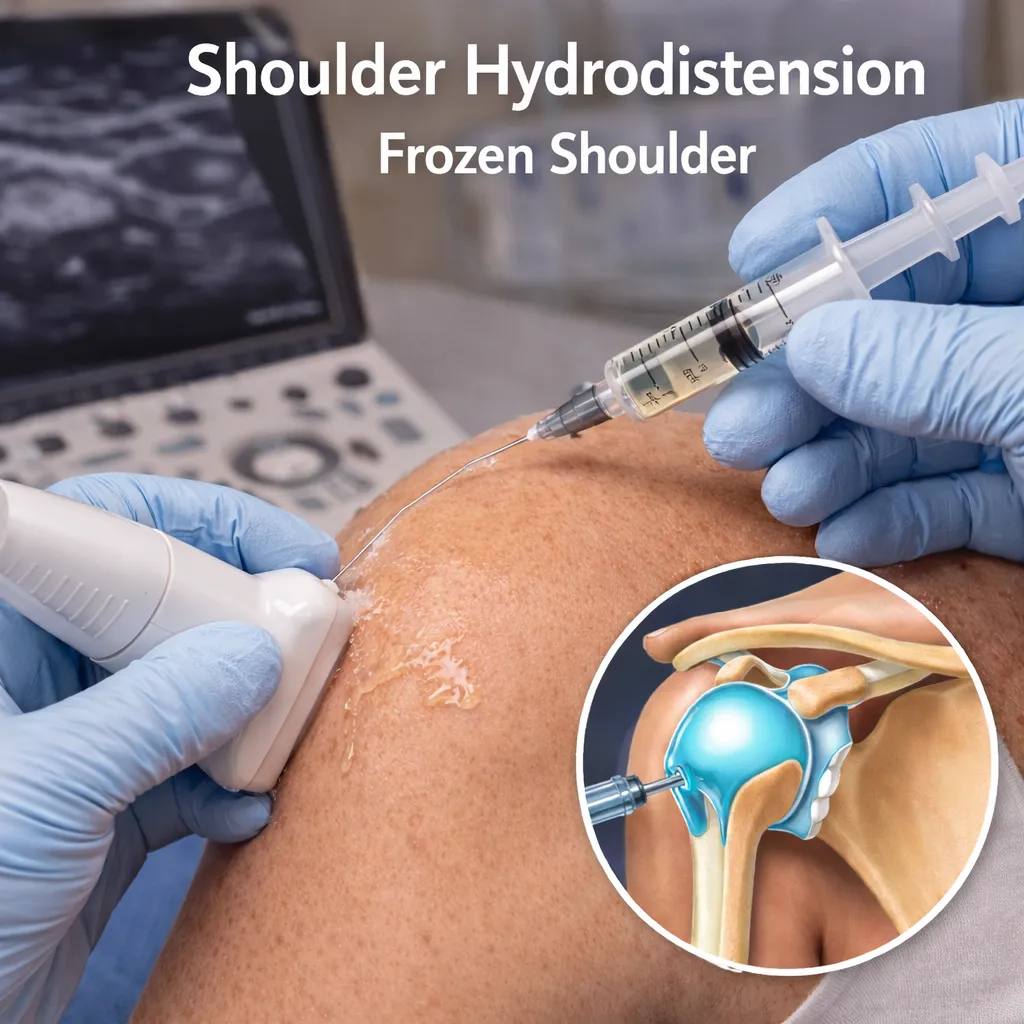
Shoulder Hydrodistension is a minimally invasive, image-guided procedure used to treat frozen shoulder (adhesive capsulitis).
What it is:
A controlled injection of sterile fluid (usually saline, often combined with local anaesthetic and anti-inflammatory medication) into the shoulder joint capsule.
What it does:
Gently stretches and expands the tight joint capsule
Breaks down adhesions and stiffness
Reduces pain and inflammation
Improves shoulder movement and function
What it’s used for:
Frozen shoulder with restricted movement
Persistent shoulder stiffness not improving with exercise alone
Accelerating recovery when combined with physiotherapy
The procedure is quick, usually performed under ultrasound guidance, and is most effective when followed by targeted physiotherapy exercises.

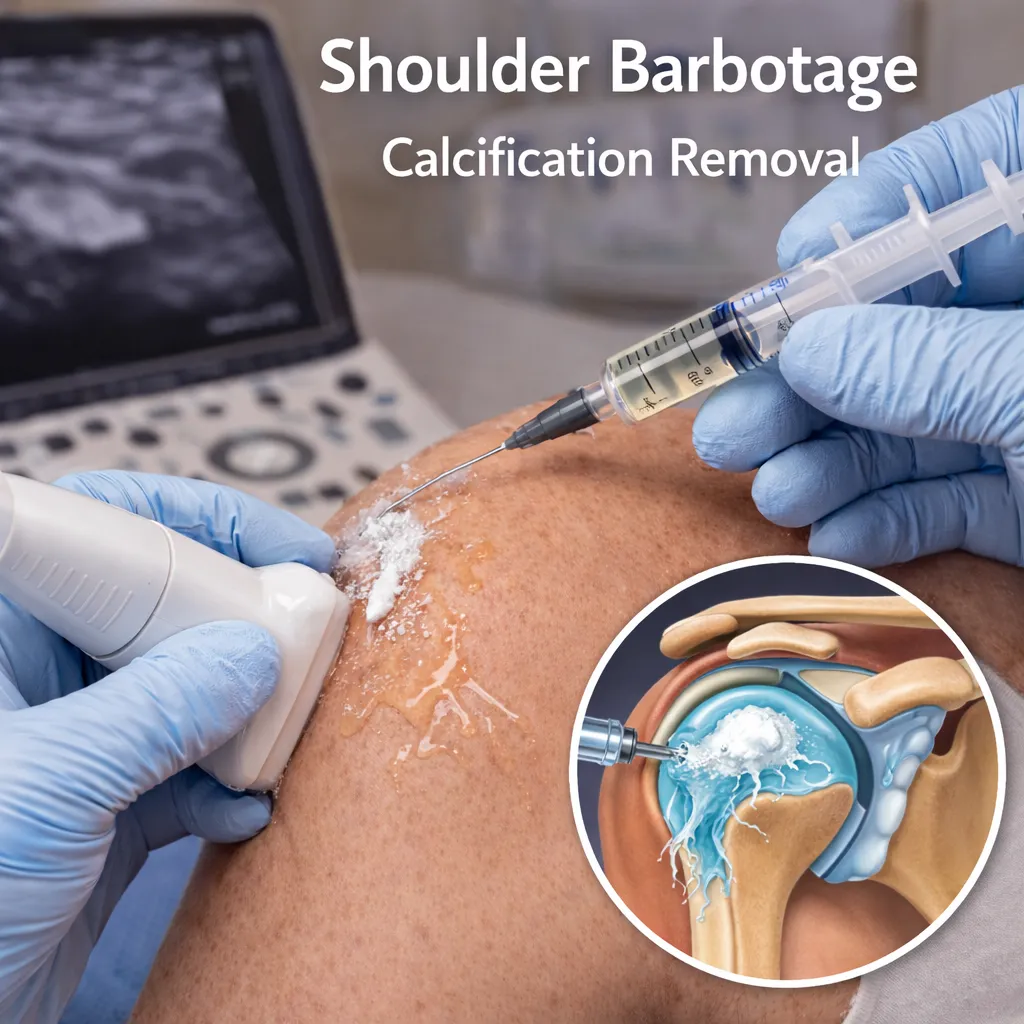
Shoulder calcification Barbotage

Shoulder Barbotage is a minimally invasive, ultrasound-guided procedure used to treat calcific tendinopathy of the shoulder.
What it is:
A specialised technique where sterile fluid is injected into the calcium deposit within a shoulder tendon to break it down and wash it out.
What it’s for:
Relieving shoulder pain caused by calcium build-up
Improving shoulder movement and function
Reducing inflammation and night pain
Avoiding or delaying surgery
When it’s used:
When shoulder pain persists despite physiotherapy
When calcium deposits are confirmed on imaging
When pain is severe, long-lasting, or disrupting sleep
When movement is significantly restricted due to calcification
The procedure is quick, precise, and most effective when followed by a structured physiotherapy programme to restore strength and mobility.
Prolotherapy
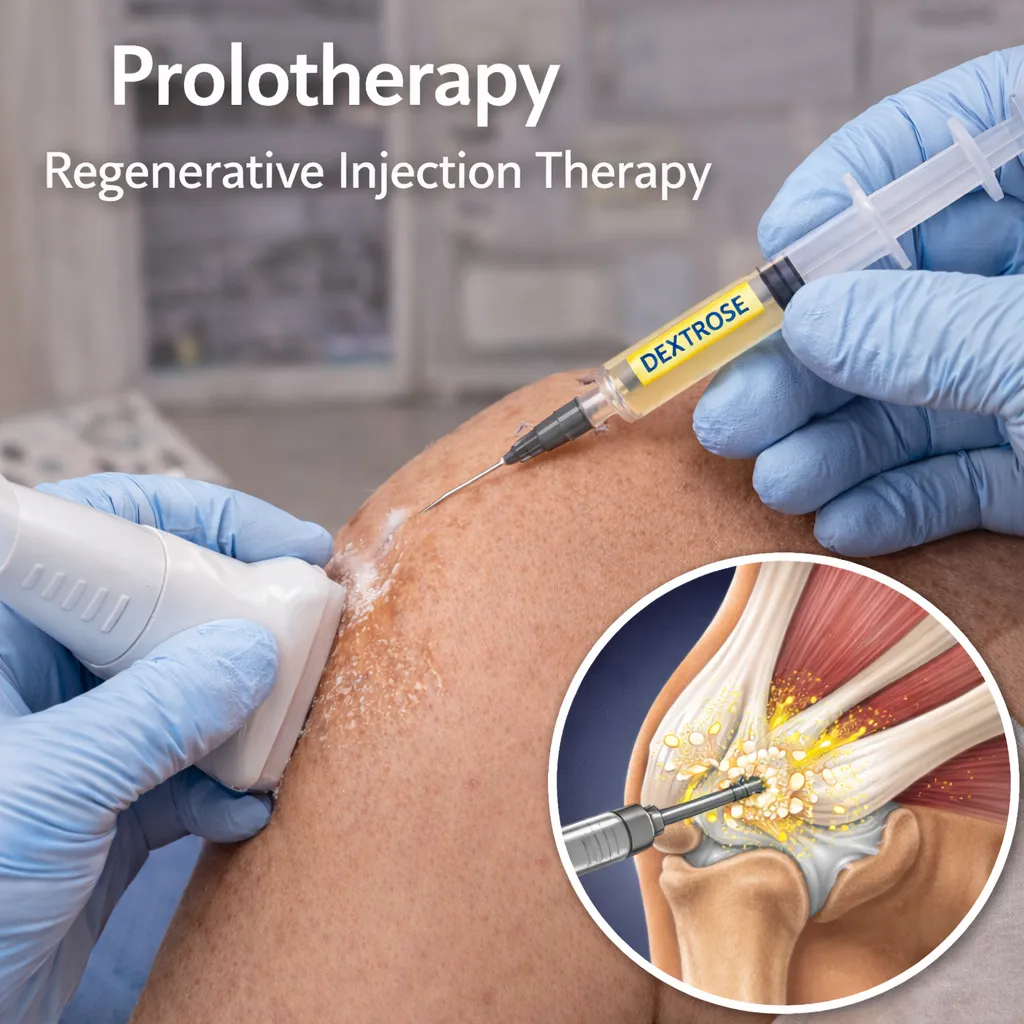
Prolotherapy is a regenerative injection treatment used to stimulate the body’s natural healing response in ligaments, tendons, and joints.
What it is:
A series of targeted injections using a natural irritant solution, typically dextrose, delivered to weakened or injured tissues to promote repair and tissue strengthening.
What it’s for:
Chronic tendon and ligament injuries
Joint instability or laxity
Persistent musculoskeletal pain
Supporting tissue healing and long-term stability
When it’s used:
When pain persists despite physiotherapy and rehabilitation
When imaging shows ligament or tendon weakness rather than inflammation
For recurrent injuries or joint instability
When a regenerative approach is preferred over steroid injections
Prolotherapy is usually delivered as a course of treatments and is most effective when combined with a tailored physiotherapy programme to restore strength, control, and function.

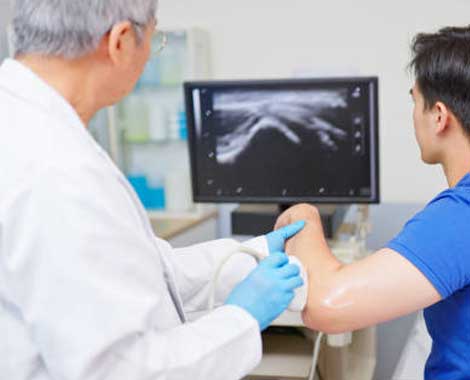
Diagnostic MSK Ultrasound Scan

Diagnostic MSK Ultrasound Scan is a non-invasive imaging test used to assess muscles, tendons, ligaments, joints, and soft tissues in real time.
What it is:
A safe, radiation-free scan that uses high-frequency sound waves to create live images of the musculoskeletal system.
What it does:
Visualises soft tissue structures in detail
Detects inflammation, tears, fluid collections, and degeneration
Allows dynamic assessment (movement during scanning)
Guides accurate diagnosis and treatment planning
What it’s used for:
- Shoulder, knee, hip, ankle, wrist, and elbow pain
- Tendon and ligament injuries
- Muscle tears and strains
- Bursitis, impingement, and joint effusions
- Guiding injections or procedures when needed
MSK ultrasound is quick, painless, and provides immediate results, making it a powerful tool for precise diagnosis and targeted treatment.
Physiotherapy & Rehabilitation
Physiotherapy and rehabilitation are a core part of both pain management and long-term recovery, whether used after injection treatments or as a stand-alone approach for musculoskeletal conditions.
What it is:
A structured, evidence-based programme of exercise therapy, movement retraining, and manual techniques, tailored to the individual and guided by a qualified musculoskeletal clinician.
What it does:
Restores strength, flexibility, and joint mobility
Improves movement patterns and biomechanics
Reduces pain and stiffness
Enhances joint stability and load tolerance
Supports tissue healing and functional recovery
Helps prevent recurrence of injury
How it helps after injections:
Injection treatments (such as steroid, hyaluronic acid, Arthrosamid, or hydrodistension) can reduce pain and inflammation — physiotherapy then maximises and prolongs the benefit of these treatments by:
Taking advantage of reduced pain to restore movement and strength
- Preventing stiffness from returning
- Improving joint control and muscle balance
- Reinforcing correct movement patterns
- Supporting long-term symptom relief rather than short-term improvement
Physiotherapy is often the key factor in translating pain relief from injections into meaningful, lasting functional improvement.
What it’s used for after injections:
- Rehabilitation following joint injections
- Restoring range of motion after hydrodistension
- Strengthening and load management after knee, shoulder, or hip injections
- Improving function and confidence in daily activities and sport
- Reducing the likelihood of symptoms returning
What it’s used for more generally:
Physiotherapy is also highly effective as a stand-alone treatment for a wide range of musculoskeletal conditions, including:
- Acute and chronic joint pain
- Sports and overuse injuries
- Tendon, ligament, and muscle injuries
- Back and neck pain
- Postural and movement-related pain
- Post-operative rehabilitation
- Injury prevention and performance optimisation
Key point:
Physiotherapy doesn’t just treat symptoms — it addresses the underlying cause of pain and dysfunction. When combined with injection therapies, it helps deliver better, longer-lasting outcomes by restoring movement, strength, and confidence.
Meet the Team of Professionals

Boobala Subramanian (BOB)
Currently, Bob serves as:
MSK Sonographer at University Hospital Coventry and Warwickshire (Coventry)
Areas of Specialisation:
Advanced assessment and diagnosis of complex MSK disorders and treatment.
Diagnostic musculoskeletal ultrasound and ultrasound-guided interventions-
Collaborative care with orthopaedics, rheumatology, neurosurgery, and pain management teams
Mentorship, training, and pathway development for advanced MSK practitioners
In addition to his clinical roles, Bob has held senior leadership positions, including Associate Clinical Director and Orthopaedic Clinical Lead, overseeing multi-site service delivery, implementing clinical governance frameworks, and mentoring extended scope practitioners (ESPs).
Advanced Physiotherapy Practitioner | MSK Diagnostic & Interventional Sonographer | Clinical Lead

Emma Johnson
Ektaa graduated with a BSc (Hons) in Podiatry from the University of Northampton, where she also distinguished herself as Vice Chair of the Students’ Union and as a student representative throughout her studies. She has trained extensively in diabetic foot care, rheumatology, dermatology, sports injuries, paediatrics, vascular, neurological, and orthopaedic podiatry, as well as soft-t
Musculoskeletal assessment & rehabilitation
Advanced nail surgery (including partial & total nail ablation under local anaesthetic)
Management of ingrown toenails with permanent surgical solutions
Acute sports injury care & prevention
Neurovascular assessment, wound care, and custom orthotic fabrication
Senior Musculoskeletal Podiatrist | Nail Surgery Specialist

Hrishikumar Ganesh
Currently, serves as:
Strength & Conditioning Coach | Sports Rehabilitation Specialist | Physiotherapy MSc (in training)
Areas of Specialisation:
Strength and conditioning for elite and professional athletes
One-to-one programme design for performance enhancement and injury rehabilitation
Sports injury management and musculoskeletal rehabilitation
Sports massage therapy for injury recovery and pain management
Integration of exercise therapy, manual therapy, and movement-based rehabilitation
Application of yoga-based practices (asana and pranayama) for musculoskeletal and long-term condition management
Hrishikumar has over seven years of experience working as a Strength and Conditioning Coach(MSc Sports Science), supporting both elite teams and professional athletes through bespoke exercise programmes aimed at improving performance and facilitating safe return to sport following injury.
He is a Level 3 qualified Sports Massage Therapist, with extensive experience using manual therapy as an effective modality for treating sports injuries and musculoskeletal conditions. His professional experience includes working with prestigious organisations such as the Board of Control for Cricket in India (BCCI), the Sports Authority of India, and the University of Bath.
Sports exercise and Strength conditioning therapist

Prashanth Gorolla
Prashanth Gorolla is an accomplished physiotherapist with expertise in musculoskeletal (MSK) care, rehabilitation, and manual therapy. With a proven track record of helping patients regain mobility, recover from injury, and improve their quality of life, Prashanth combines advanced clinical skills with a patient-first philosophy.
Currently based in Oxford, Prashanth serves as a Senior MSK Clinician at Connect Health now Cora Health, where he provides specialist assessment, evidence-based treatments, and personalised rehabilitation plans for patients with a wide range of MSK conditions.
Musculoskeletal assessment & rehabilitation
Manual therapy techniques
Post-injury & post-operative recovery
Exercise prescription and mobility training
Patient-centred education and prevention strategies
Senior Musculoskeletal Physiotherapist | Chartered Society of Physiotherapy Member | HCPC Registered Clinician
Curious about Pricing?
Click “Book Your Appointment Now” to view clear, upfront pricing for each procedure/treatment.
General – FAQs
Answers to Your Top Questions at GB Clinics
Do I need a referral to book an appointment?
No. You can book directly for any of our services by clicking on the button "Book your appointment now".
How do I book an appointment?
You can book through our online booking system, by clicking the button "Book your appointment now"
Do you accept health insurance?
Yes — we work with most major insurance plans, specifics might depends on your specific insurer.
What should I bring to my first appointment?
Please bring any relevant medical reports, imaging results, a list of current medications, and your insurance or payment information. The clinician will review your history before your assessment.
What happens during my first visit?
Your first appointment includes a detailed discussion of your symptoms and medical history, followed by a thorough physical assessment. Where appropriate, diagnostic imaging (such as MSK ultrasound) is performed during the same visit and used in conjunction with the specific injection or procedure to ensure accuracy and optimal treatment outcomes.
Do you also offer Physiotherapy & Rehabilitation as required?
Yes, we offer specialist Physiotherapy and Rehabilitation to help accelerate recovery and further enhance the results of any of the procedures listed above. In addition, we provide a comprehensive range of physiotherapy treatments to support the assessment and management of musculoskeletal (MSK) conditions.
Injections – FAQs
Steroid(Cortisone) Injections, how quickly do they work?
Some patients experience relief within 48–72 hours, while others notice gradual improvement over 1–2 weeks. In some cases, pain may briefly increase before settling.
Are cortisone injections painful?
Discomfort is usually mild and brief. Local anaesthetic is commonly used, and ultrasound guidance improves accuracy and comfort.
Hyaluronic Acid (HA) Joint Injections, how long do the effects last?
Relief can last several months, depending on the joint and severity of degeneration. The clinician will be able to give you better advice based on your assessment.
Shoulder procedures – FAQs
(Hydrodistension& Calcification Barbotage)
What is shoulder Hydrodistension? Is it safe?
A targeted, minimally invasive procedure that gently stretches the shoulder joint capsule by injecting sterile fluid under imaging guidance to improve pain and range of motion for frozen shoulder (adhesive capsulitis).
Hydrodistension is generally low risk, with minimal side effects such as mild soreness or temporary swelli
Can I drive or work after a procedure?
Most patients can resume light activities soon after, but avoid heavy lifting or strenuous use of the treated area for a few days. Specific advice depends on the procedure and your recovery plan.
Shoulder Calcification Barbotage. What symptoms does it treat? Is it better than surgery?
It helps relieve severe shoulder pain, night pain, and restricted movement caused by calcific tendinopathy. In many cases, barbotage avoids the need for surgery and speeds up recovery.
Ganglion (Cyst) Aspiration – FAQs
Will the cyst come back after aspiration?
Recurrence is possible, but aspiration often reduces symptoms and may prevent the need for surgery. We will also, make sure to provide you with advice to avoid recurrence.
Is the procedure painful?
Local anaesthetic is used, and discomfort is usually minimal.
Diagnostic MSK Ultrasound Scan – FAQs
What does an MSK ultrasound scan show?
It provides real-time images of muscles, tendons, ligaments, joints, bursae, and soft tissues, helping identify inflammation, tears, fluid, or degeneration.
Is ultrasound better than X-ray or MRI?
Ultrasound excels at soft tissue assessment and allows dynamic movement during scanning. It can often be performed immediately without waiting times.
Is it painful or harmful?
No. It is painless, radiation-free, and completely safe.
Prolotherapy – FAQs
What conditions is it used for?
It is commonly used for chronic joint instability, tendon injuries, and persistent musculoskeletal pain.
How many sessions are needed?
Most patients require a course of treatments spaced several weeks apart, depending on the condition.